A confident smile reflects one’s personality and is crucial to overall well-being. However, dealing with missing teeth and achieving that confidence can be challenging for many individuals. The impact of missing teeth extends beyond aesthetics, affecting oral health and self-esteem. This guide aims to shed light on the significance of restoring missing teeth and explore the various options available to achieve this goal.
The Causes of Missing Teeth
Tooth loss may happen due to various causes, such as poor oral hygiene, accidents, or medical conditions. One primary reason is dental decay, which is caused by bacteria in the mouth that produce acids. These acids erode the enamel, causing cavities. Untreated decay can get deeper into the tooth, resulting in infection and eventual loss.
Periodontal or gum disease is a common cause of tooth loss. This condition affects the oral tissues surrounding the teeth, leading to inflammation and damage in the gums and jaw bones. If left untreated, the disease can cause teeth to loosen and fall out.
Traumatic injuries, such as sports injuries, falls, or vehicle accidents, can also result in tooth loss. The impact of a forceful blow can fracture or dislodge teeth, necessitating their extraction or replacement.
Additionally, certain medical conditions and habits can contribute to tooth loss. These include untreated bruxism (teeth grinding), which can wear down tooth enamel over time, and systemic diseases such as diabetes or osteoporosis, which can weaken the bone supporting the teeth.
Understanding the Consequences of Missing Teeth
Missing teeth can significantly impact one’s appearance, oral health, and well-being. By better understanding these consequences, one can realize the importance of seeking appropriate treatment for tooth loss.
Impact on Oral Health
Missing teeth can have detrimental effects on oral health, primarily because they reduce stimulation to the jawbone and surrounding structures.
- Bone Loss: With tooth loss, the alveolar bone that once supported it undergoes resorption, a process in which the bone gradually diminishes in volume and density. The bone deteriorates without a tooth root to stimulate the jawbone through chewing and biting forces. Losing bone density weakens the overall bone structure, potentially leading to facial collapse and prematurely ageing appearance.
- Shifting of Surrounding Teeth: The absence of a tooth can disrupt the balance of forces within the mouth, causing neighbouring teeth to drift or tilt into the vacant space. This phenomenon, known as dental drift, can result in misalignment issues, changes in bite alignment, and potential complications with jaw function. Over time, dental drift may necessitate orthodontic intervention to realign the teeth and restore proper occlusion.
- Difficulty Chewing: Missing teeth can compromise the ability to chew food effectively, leading to problems breaking down food particles and initiating the digestive process. As a result, individuals may experience discomfort while eating and a reduced ability to extract essential nutrients from their diet, contributing to nutritional deficiencies, digestive issues, and an overall decline in health and well-being.
Aesthetic Concerns
Missing teeth can significantly impact one’s appearance and self-confidence, leading to aesthetic concerns that extend beyond the physical gap in the smile.
- Gaps in the Smile: The visible absence of teeth can create noticeable gaps in the smile, disrupting the harmony and symmetry of facial features. Individuals may feel self-conscious about their appearance and avoid smiling or speaking in social situations, leading to social withdrawal and diminished quality of life. Additionally, gaps in the smile can affect speech articulation, further exacerbating communication challenges.
- Changes in Facial Structure: Missing teeth cause hollowness in the overlying facial features, leading to sagging and asymmetry.
Functional Challenges
Losing teeth can pose significant functional challenges, affecting speech clarity, chewing, and oral function.
- Difficulty Speaking: Missing teeth, especially those in the anterior region of the mouth, can impair the ability to articulate certain sounds properly, leading to speech impediments and communication difficulties. Individuals may need help with pronunciation, clarity, and confidence in their speech, impacting social interactions and professional communication.
- Impaired Chewing Function: Missing teeth can compromise the efficiency and effectiveness of the chewing process, making it challenging to bite and tear food into smaller, digestible pieces. This can result in discomfort, frustration, and even avoidance of certain foods that require extensive chewing. Over time, dietary restrictions and compromised chewing function lead to nutritional deficiencies and weight loss.
Options for the Treatment of Missing Teeth
Several options for missing teeth restoration are available, such as dental implants, dentures, and dental bridges. Each choice offers unique advantages and has certain requirements, which are discussed in detail as follows:
Dental Implants
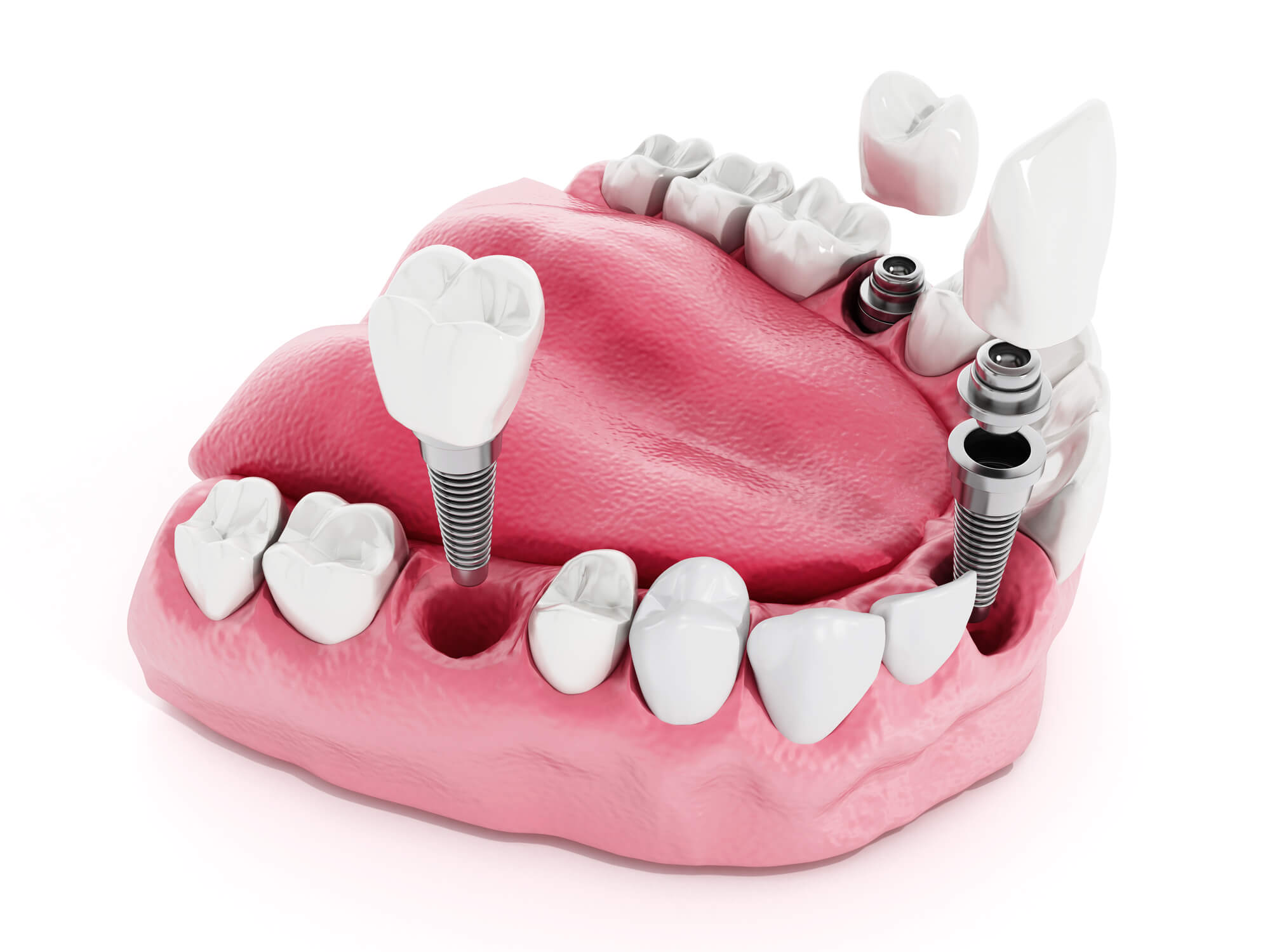
Dental implants consist of small, biocompatible titanium posts surgically inserted into the jawbone. This process requires precision and expertise, as the implants must be strategically placed to ensure optimal support and stability for the replacement teeth. Once the implants are in position, they gradually fuse with the surrounding bone through osseointegration, which creates a strong bond between the jawbone and the implant, mimicking the natural relationship between tooth roots and bone.
The Dental Implants Process
Firstly, the patient’s oral health, including X-rays and digital scans, is evaluated to assess bone density. Dental implants are then surgically positioned into the jawbone by a qualified oral surgeon. Following implant placement, a healing period is necessary for osseointegration, during which the implants fuse with the surrounding bone tissue. Once osseointegration is complete, abutments are attached to the implants, which connect the replacement teeth. Finally, custom-made dental crowns, bridges, or dentures are fabricated to match the patient’s natural teeth and attached to the implants, restoring function, aesthetics, and confidence in the smile.
Types of Dental Implants
Several types of dental implants are available, each designed to meet specific needs and preferences:
- Endosteal Implants: they are the most commonly used type of dental implant. They are inserted directly into the jawbone, where they fuse with the surrounding bone tissue. Endosteal implants are best suited for individuals with sufficient bone density and healthy gums, providing a stable and durable foundation for replacement teeth.
- Subperiosteal Implants: Subperiosteal implants are a great option for individuals with insufficient bone density to support endosteal implants. Instead of being inserted in the jawbone, subperiosteal implants are placed on top of the bone beneath the gum tissue. This type of implant may be recommended for individuals with jawbone resorption or other anatomical limitations.
- Zygomatic Implants: Zygomatic implants are a unique type of dental implant used in cases where traditional implants may not be possible due to severe bone loss in the upper jaw. Instead of anchoring the implants in the maxillary bone, zygomatic implants are anchored in the zygomatic (cheek) bone, providing a stable foundation for replacement teeth.
Benefits of Dental Implants
- Permanent Solution: Dental implants offer long-term stability and durability, unlike traditional dentures or bridges, which may require replacement or adjustment over time. This permanence enhances the functionality of the replacement teeth and provides peace of mind for individuals seeking a reliable solution.
- Resemblance to Natural Teeth: Dental implants closely mimic the look, feel, and function of natural teeth. The replacement teeth, custom-designed to match the surrounding teeth’ shape, color, and alignment, blend seamlessly into the smile. This natural appearance allows individuals to smile, speak, and chew normally.
- Support Jaw Bone: Another significant advantage of dental implants is their ability to prevent jaw bone loss. Dental implants stimulate the jawbone, which promotes bone growth and density. This preservation of bone structure maintains facial aesthetics and helps prevent complications such as jawbone atrophy and facial sagging.
Key Considerations for Dental Implants
- Adequate Bone Density: While dental implants offer numerous benefits, several considerations must be made when considering this treatment option. One primary requirement for successful implant placement is adequate bone density in the jaw. The jawbone must be strong and healthy enough to support the implants and withstand the chewing forces exerted during daily activities. In cases where bone density is insufficient, bone grafting or other preparatory procedures may be necessary to enhance the implant’s stability.
- Gum Health and Oral Hygiene: Implant placement requires healthy gums and good oral health. Conditions such as gum disease or untreated dental infections can jeopardize the success of the implants and may need to be addressed before treatment can proceed. Maintaining proper oral hygiene habits, including regular brushing, flossing, and professional cleanings, is essential for the long-term success of dental implants.
- Time: It is important to recognize that receiving dental implants involves multiple stages and requires patience and commitment from the patient. The treatment timeline may span several months, from consultation and implant surgery to the attachment of the replacement teeth.
Dental Bridges
Dental bridges are reliable solutions for individuals dealing with the challenges of missing teeth. They effectively bridge the gap left by one or more missing teeth. These prosthetic devices consist of artificial teeth, known as pontics, anchored securely to the adjacent natural teeth or dental implants.
The Process of Dental Bridges
To attach the dental bridge, the adjacent teeth are altered by removing some enamel to accommodate dental crowns, which will serve as anchors. Impressions of the prepared teeth and surrounding oral structures are then taken to create a custom-made bridge in a dental laboratory. During fabrication, the bridge is crafted to match the shape, size, and colour of the natural teeth. Once the bridge is ready, it is carefully cemented onto the prepared teeth, effectively filling in the gap left by the missing teeth.
Types of Dental Bridges
Dental bridges come in various types, each designed to address specific needs and preferences:
- Traditional Bridges: Dental bridges are a common solution for replacing missing teeth. They consist of false teeth (called pontics) anchored in position by dental crowns. These crowns are placed over natural teeth on either side of the gap, providing support and stability for the bridge.
Traditional bridges are known for their durability and natural-looking appearance and can be used to replace one or more missing teeth.
- Cantilever Bridges: Instead of being supported by dental crowns placed on healthy teeth on both sides of the gap, cantilever bridges are anchored to adjacent teeth on only one side. This type of bridge is typically used when only one healthy tooth is available adjacent to the gap.
- Maryland Bridges: Maryland bridges, also known as resin-bonded bridges, are a conservative approach to traditional bridges. Instead of using dental crowns to support the pontic, Maryland bridges use metal or porcelain wings bonded to the back of adjacent teeth. This minimally invasive option is ideal for restoring front teeth with minimal alteration to the adjoining natural teeth.
Benefits of Dental Bridges
- Restored Function: Individuals with missing teeth often struggle chewing certain foods and may experience difficulty articulating certain sounds. Bridges facilitate smoother chewing and more articulate speech by restoring the arch and filling in the gaps created by missing teeth.
- Enhanced Aesthetics: Dental bridges offer a significant aesthetic benefit by filling in the gaps and creating a seamless smile. The visible absence of teeth can impact one’s appearance and self-esteem, leading to feelings of self-consciousness and insecurity. Bridges effectively address these concerns by restoring the natural contours of the smile, boosting self-confidence, and enhancing overall facial aesthetics.
- Preservation of Tooth Alignment: When a tooth is lost, the surrounding teeth may gradually shift out of position, leading to misalignment and bite problems. By filling the gap with a bridge, adjacent teeth are stabilized and prevented from drifting, thus maintaining proper alignment and bite. This preservation of tooth alignment helps prevent potential complications such as TMJ disorders and uneven wear on the teeth.
Key Considerations for Dental Bridges
- Oral Health of Adjacent Teeth: Dental bridges can be quite beneficial, but it’s important to consider the health and strength of the adjacent natural teeth. These neighboring teeth are critical in supporting the bridge, so they must be in good condition and structurally sound. Sometimes, the adjacent teeth require reshaping or alteration to accommodate the dental crowns that act as anchors for the bridge. This preparatory step ensures a secure and stable foundation for the bridge and promotes long-term success.
- Potential for Decay and Gum Disease: Maintaining oral hygiene is essential for the longevity of a dental bridge. Without diligent care, there is a risk of decay and gum disease developing around the bridge and beneath the dental crowns. Regular brushing, flossing, and dental check-ups are essential for removing plaque and bacteria, preventing inflammation of the gums, and preserving the integrity of the supporting teeth. Additionally, individuals with bridges may benefit from specialized oral hygiene tools such as water flossers and interdental brushes to ensure thorough cleaning around the prosthetic teeth and under the bridge.
- Longevity: Dental bridges are meant to be durable and long-lasting, but they may require replacement over time due to wear and tear. A bridge’s lifespan depends on various factors, including the materials used, the individual’s oral hygiene habits, and the forces exerted during chewing and speaking. With care and maintenance, regular dental check-ups, and professional cleanings, bridges can provide reliable function and aesthetics for many years.
Removable Dentures
Removable dentures have long served as a traditional yet effective solution for individuals with missing teeth. These prosthetic devices offer a customizable remedy that restores function and aesthetics, allowing wearers to regain their smiles and oral function.
The Process of Removable Dentures
Obtaining removable dentures involves several steps to ensure a comfortable fit and natural appearance. A comprehensive examination of the mouth, including impressions, measurements, and digital scans, is conducted to create a customized treatment plan. Next, any remaining teeth that will serve as anchor points for the denture are prepared, and impressions of the oral structures are taken to create a precise mould. Based on these impressions, the dental laboratory fabricates a trial denture for the patient to evaluate fit, function, and aesthetics. Adjustments are made as necessary to achieve optimal comfort and appearance. Once the final denture is ready, it is placed in the mouth, and the patient receives instructions on proper care and maintenance.
Types of Removable Dentures
Removable dentures come in various types, each tailored to address specific needs and preferences:
- Full Dentures: Full dentures replace all teeth in the upper or lower arch. These dentures consist of artificial teeth set in a gum-coloured acrylic base that rests directly on the gum. They are crafted to mimic the appearance and function of natural teeth, enabling wearers to eat, speak, and smile normally.
- Partial Dentures: For individuals with a few missing teeth who wish to restore their full dentition, partial dentures are a great option. These dentures consist of prosthetic teeth on a metal or acrylic base that blends seamlessly with the natural gums. They are customized to fit comfortably alongside the remaining natural teeth, providing a seamless and functional solution.
Benefits of Removable Dentures
Removable dentures offer several benefits for individuals with missing teeth:
- Affordability: Removable dentures are a cost-effective solution for restoring a smile, making them accessible to many individuals.
- Versatility: Unlike fixed dental prosthetics such as implants or bridges, dentures can be easily removed for cleaning and maintenance. This versatility allows wearers to maintain optimal oral hygiene and address discomfort or irritation.
- Customization: Removable dentures are highly customizable, allowing for precise adjustments to ensure a comfortable and natural fit. Dentists work closely with patients to create dentures that complement their facial features, enhance their smiles, and restore their confidence.
Key Considerations for Removable Dentures
While removable dentures offer numerous benefits, there are several considerations to keep in mind:
- Stability: Some wearers may experience challenges related to stability, particularly during activities such as eating or speaking. However, advances in denture technology have led to the development of adhesives and suction mechanisms that enhance stability and comfort.
- Maintenance: Proper care is extremely important for the longevity and effectiveness of removable dentures. Denture wearers must adhere to a strict oral hygiene regimen, including daily cleaning and regular dental check-ups. Additionally, dentures may require periodic adjustments, relining, or replacement to accommodate changes in the mouth’s structure over time.
- Adaptation Period: It is common for individuals to experience an adjustment period when transitioning to removable dentures. Initially, wearers may notice changes in speech or chewing function as they become accustomed to the new prosthetic. However, with patience and practice, these challenges typically diminish, allowing wearers to enjoy the full benefits of their dentures.
Implant-Supported Dentures
Implant-supported dentures, also known as overdentures, combine the stability and strength of dental implants with the feasibility of removable dentures. These prosthetic devices consist of artificial teeth attached to a base that snaps onto dental implants surgically placed in the jawbone. The dental implants serve as sturdy anchors, securely holding the dentures in place and preventing slippage or discomfort during daily activities.
The Process of Implant-Supported Dentures
Implant-supported dentures involve surgically placing dental implants into the jawbone. These titanium implants serve as artificial tooth roots, providing a solid anchor to which the dentures can attach. The number and location of implants depend on the individual’s needs and the type of denture used. After implant placement, a healing period allows the implants to merge with the surrounding bone tissue through a process called osseointegration.
Once osseointegration is complete, the custom-designed dentures are fabricated to fit securely over the implants. These dentures are crafted to blend seamlessly with the natural teeth and gums, providing a lifelike appearance and comfortable fit. The dentures are then attached to the implants using connectors called snaps, ensuring a secure and stable hold.
Types of Implant-Supported Dentures
Implant-supported dentures come in several types, each offering unique advantages and considerations tailored to individual needs and preferences. The primary types include:
- Bar-Retained Dentures: In this type, a metal bar is attached to dental implants placed in the jawbone. The denture is then secured to the bar using clips or attachments, providing stability and support while allowing for easy removal for cleaning.
- Ball-Retained Dentures (Locator Attachment): Ball-retained dentures utilize a ball-and-socket mechanism to secure the denture to the implants. The implants feature a ball-shaped attachment that fits into sockets on the denture, creating a secure and stable connection that prevents slippage and movement.
- All-on-4 or All-on-6 Dental Implants: These procedure involve four or six dental implants strategically positioned within the jawbone to support a full arch of replacement prosthetic teeth. This approach offers maximum stability and eliminates the need for bone grafting in many cases, making it ideal for individuals with extensive tooth loss or compromised bone density.
- Fixed Implant-Supported Dentures: Fixed implant-supported dentures are permanently attached to dental implants, providing a permanent solution for missing teeth. Unlike removable dentures, fixed dentures cannot be removed by the wearer and are securely anchored in place, offering enhanced stability and functionality.
- Removable Implant-Supported Dentures: Removable implant-supported dentures combine the stability of dental implants with the convenience of removable dentures. These dentures feature attachments that snap onto implants, providing a secure hold while allowing for easy removal for cleaning and maintenance.
Benefits of Implant-Supported Dentures
- Enhanced Stability: Implant-supported dentures offer enhanced stability compared to traditional dentures. Wearing these dentures anchored to dental implants provides wearers with increased confidence and comfort, as the prosthetic teeth remain securely in place during daily activities such as speaking and chewing.
- Improved Chewing Efficiency: Implant-supported dentures offer improved chewing efficiency, allowing wearers to enjoy a varied diet without restrictions. The stable foundation provided by dental implants enables better distribution of biting forces, enhancing the ability to chew tough or crunchy foods easily.
- Preservation of Bone Density: Another notable advantage of implant-supported dentures is their ability to preserve bone density in the jaw. Unlike traditional dentures, which can contribute to bone resorption over time, implant-supported dentures stimulate the underlying bone, helping to maintain its strength and density. This preservation of bone structure can prevent facial collapse and maintain facial aesthetics.
Key Considerations for Implant-Supported Dentures
While implant-supported dentures offer numerous benefits, there are also some considerations to keep in mind:
- Adequate Bone Density: While implant-supported dentures offer numerous benefits, they require sufficient bone density for successful implant placement. Patients with inadequate bone volume may need bone grafting or other preparatory procedures to augment the jawbone and create a suitable foundation for the implants. Patients with severe bone loss may not be eligible for implant-supported dentures and may need to explore alternative treatment options.
- Treatment Timeline: Receiving implant-supported dentures involves multiple stages, including implant placement, healing, and fabrication. As a result, the treatment timeline may be longer than that of other tooth replacement options.
- Cost: Implant-supported dentures require a higher initial investment, but they are a long-term investment in oral health and quality of life.
Factors in Choosing Missing Teeth Treatment
Selecting the most suitable treatment for missing teeth is a significant decision that requires careful consideration of various factors. Several aspects are crucial in determining the optimal treatment approach, from the number of missing teeth to individual lifestyle preferences. By evaluating these factors with a qualified dentist’s guidance, individuals can effectively make informed decisions that address their unique needs and preferences.
Number of Missing Teeth
The number of missing teeth is a fundamental factor significantly influencing treatment choice. Whether it’s a single missing tooth, multiple teeth, or an entire arch, the extent of tooth loss dictates the appropriate treatment approach. For individuals with a single missing tooth, options such as dental implants or a traditional bridge may be suitable. Conversely, extensive tooth loss may necessitate solutions like implant-supported dentures or full arch implants. By assessing the specific number and location of missing teeth, dentists can tailor treatment plans to meet individual needs.
Oral Health
The overall oral health of an individual determines the feasibility of different treatment options. Key aspects such as the condition of the remaining teeth, gum health, and bone density are considered. For example, individuals with healthy gums and sufficient bone density may be candidates for dental implants, which require adequate support from surrounding tissues. Conversely, individuals with gum disease or significant bone loss may benefit from alternative options such as removable dentures or bridges. Dentists evaluate oral health status through comprehensive examinations, including dental X-rays and periodontal assessments, to determine the most appropriate treatment approach.
Existing Medical Conditions
Existing medical conditions can also influence the choice of treatment for missing teeth. Certain health conditions, such as diabetes mellitus or autoimmune disorders, may affect the body’s ability to heal properly after dental procedures. Additionally, medications taken for chronic conditions may have implications for dental treatment. By addressing medical considerations upfront, dentists can develop treatment plans that prioritize patient safety and well-being.
Lifestyle Factors
Lifestyle factors and personal preferences play a significant role in determining the most feasible treatment for missing teeth. Budget, desired treatment timeline, and willingness to undergo surgical procedures can influence treatment decisions. For example, dental implants may offer long-term benefits but require a higher initial investment and a longer treatment timeline than removable dentures. Additionally, some individuals may prefer the convenience of removable dentures, which are removable for cleaning and maintenance. By considering lifestyle factors and preferences, dentists can recommend treatment options that align with each patient’s unique circumstances and goals.
Cosmetic Concerns
Maintaining a good appearance is crucial for many people seeking treatment for missing teeth. How their smile looks significantly affects their self-confidence and overall well-being. In dental restorations, restoring functionality and ensuring that the prosthetic teeth blend seamlessly with the natural teeth to achieve the best aesthetic results is important. Dentists use advanced techniques and materials to create prosthetic teeth that resemble natural teeth in color, shape, and alignment. Whether a person opts for dental implants, bridges, or dentures, they can get a restored smile that enhances their confidence and quality of life.
Conclusion
In conclusion, selecting the appropriate treatment for missing teeth entails a comprehensive evaluation of factors such as the extent of tooth loss, oral health status, existing medical conditions, lifestyle preferences, and aesthetic considerations. Collaborating with a qualified dentist facilitates personalized treatment plans. Whether contemplating dental implants, bridges, or dentures, these options offer avenues for enhancing oral health and overall well-being. Through consultations with dental experts, individuals can make informed decisions, leading to effective restoration of their smiles and improved quality of life. To book a free consultation with our dental team, contact us Bay Area Implant Dentistry , a premier clinic located in Fremont, California today!